
The Haematology Institute Nurses and Allied health Professionals Group is hosting a one day event on 10th July 2017 at the Robens Suite, 29th floor, Tower Wing, Guy’s Hospital London […]
Read full story
The Haematology Institute Nurses and Allied health Professionals Group is hosting a one day event on 10th July 2017 at the Robens Suite, 29th floor, Tower Wing, Guy’s Hospital London […]
Read full story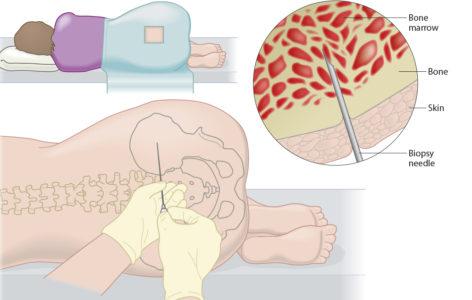
Until now, bone marrow sampling has been the primary technique for routine follow-up checks on MDS patients after initial diagnosis. The bone marrow is the heart of the disease and […]
Read full story
The Cancer Drug Fund (CDF) de-listing further drugs Many blood cancer patients are about to face more severe issues of access to treatment, following the announcement that the CDF is […]
Read full story
19th Congress of the European Haematology Association (EHA) has taken place this year between 12th and 15th June in Milan, Italy. This event is set up for physicians and representatives […]
Read full story